Overview
Has your dentist diagnosed you with condensing osteitis? Perhaps, you have never heard about it before. You are probably here to know more about the concerned dental health condition.
At TruCare General Dentistry Roswell, GA, we have helped several patients with the condition so far. Here, we will answer all the queries about condensing osteitis that our surgeons come across. Let’s start with the basics.
Focal sclerosing osteitis
Condensing osteitis or focal sclerosing osteitis is a periapical inflammatory condition. Dentists notice abnormal bone growth and lesions in affected molars on the jawbone. The disease often impacts the bone next to teeth that have undergone endodontic therapy or restored with other techniques.
Patients might experience mild pain in some instances. Thankfully, the condition is localized. Therefore, it does not spread to other parts of the individual’s mouth.
Though there are no significant symptoms, the condition can quickly harm the affected teeth. It’s also considered one of the types of jaw lesions. Therefore, in severe cases, dentists start the treatment immediately post-diagnosis.
Diagnosis
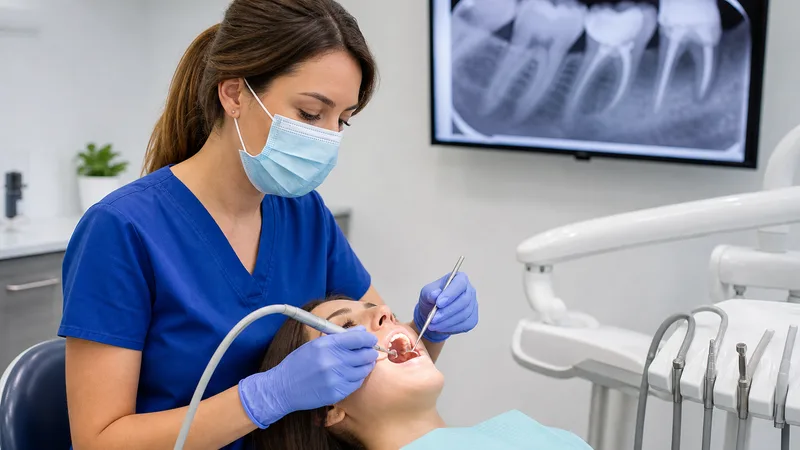
The diagnosis part is a bit tricky due to the asymptomatic nature of this condition. Most cases of focal sclerosing osteitis are diagnosed during routine dental checkup x-rays. However, it’s a rare condition and makes up only 2 percent of patients diagnosed during x-ray examination.
X-rays do allow surgeons to inspect bony areas. However, jawbone growths or tumors can indicate other issues besides condensing osteitis. Therefore, your dentist can recommend a biopsy on specific bone lesions if necessary.
Some patients may need root canals. So, your dental clinic might refer you to an endodontist.
What triggers condensing osteitis?
The surprising aspect is that even individuals who follow proper oral hygiene habits can face focal sclerosing osteitis.
The condition is a sclerotic reaction. It is triggered due to a combination of bacteria with a low degree of virulence and the immune system’s response to the infection in the tooth root.
Scientists consider it as a sort of inflammatory stimulus. A wide range of infections and dental pulp inflammation can cause this oral health condition. In addition, dental care experts come across cases that link the dental disease with chronic root canal inflammation.
Patients with a superb immune system are more prone to condensing osteitis. When it comes to highlighting the age group, most patients are young or older adults. Yet, there’s a lack of clarity on numbers as most asymptomatic cases go unreported.
Treatment options
The aim is to wholly or partially treat the lesion gradually. The treatment consists of surgical debridement and antibiotics to eliminate the infection and provide symptomatic relief.
Post-diagnosing condensing osteitis, your dental clinic will refer your case to an endodontist. However, some clinics do have in-house experts.
First, your endodontist will closely examine the affected tooth to find the underlying cause. Then, in case of the presence of infection, your dentist will prescribe antibiotics to ease the inflammation.
Dental care professionals prefer taking a slower approach for asymptomatic cases. If the person’s condition progresses with antibiotics, the treatment becomes easy.
The second step is to test the pulp present inside the infected tooth. So, professionals will conduct a VPT (vital pulp test). There is no other alternative to tooth extraction if the pulp shows signs of irreversible pulpitis. The same is the case if tooth pulp has turned necrotic.
If the damage is recoverable, dentists recommend a root canal treatment. The procedure is painless and enjoys a high success ratio. Plus, it takes care of the lesions, inflammation, and any infection present in the tooth. However, post-procedure checkups (x-rays) remain crucial to ensure the operated tooth remains healthy.
No matter if your dentist recommends root canal or extraction. Your surgeon will start the treatment after treating the present infection with antibiotics.
Does condensing osteitis indicate a failed root canal therapy?
Well, studies do indicate the possibility. As per Taiwanese scientists, most condensing osteitis cases involve inadequately treated endodontic problems. Put simply, failed root canal therapy can lead to problems.
The same research indicates that proper root canal therapy and obturation decrease condensing osteitis lesions. However, the condition does not subside if formed due to a failed root canal. Then, the only option is tooth extraction.
Which teeth are most affected due to focal sclerosing osteitis?
The most-reported ones are the apex of premolars and molars in the lower jaw.
To conclude:
There is nothing much to be done in case of an overreacting immune system. Yet, the best you can do is follow a proper oral hygiene routine. Don’t skip quarterly checkups; opt for x-rays if your dentist suggests so.
Are you experiencing pain in an old root canal tooth? Visit TruCare Dentistry in Roswell(Ga), let us examine your teeth for potential issues.
“Good oral hygiene and professional care reduce the risk of cavities, gum disease, and tooth loss over a lifetime.”
“Regular dental visits help prevent disease and catch problems early when treatment is simpler and less costly.”
Frequently Asked Questions
Does TruCare Dentistry offer general dentistry? +
Yes. TruCare Dentistry provides general dentistry for patients in Roswell, Marietta, and East Cobb.
How do I schedule an appointment? +
Call (678) 321-7575 or use our online contact form. We are located at 9205 Coleman Rd, Suite 200, Roswell, GA 30075.
Do you take dental insurance? +
We accept most major dental insurance plans. Call (678) 321-7575 and our team will confirm your coverage before your visit.
Do you see patients from Roswell and Marietta? +
Yes. Most of our patients come from Roswell, Marietta, and nearby zip codes such as 30075, 30076, 30350, 30062, and 30068. We also welcome new patients from across the greater Atlanta metro — many of our long-term patients travel from well outside the immediate area.
Do you offer same-day emergency appointments? +
Yes, during business hours we offer same-day emergency dental care when urgent pain, swelling, or trauma requires immediate attention.
Who provides care at TruCare Dentistry? +
Dr. Toral Ardeshna, DDS, and our experienced team provide personalized family, cosmetic, and restorative dentistry under one roof.
Schedule Your Visit in Roswell, GA
Same-day emergency appointments available. Serving Roswell, Marietta, and East Cobb.